Atopic skin: knowing how to take care of it and living better with it

Topicrem celebrates its 30th anniversary!
0,00€
Perhaps you are one of the 2.5 million French people¹ who suffer from atopic dermatitis, this skin condition more commonly known as eczema?
Atopic dermatitis is a chronic inflammatory skin disease that can develop at any age, and whose symptoms truly affect the quality of life! Intense itching and extreme dryness make daily life difficult. Although the symptoms can be bothersome, steps can be taken to improve quality of life. Despite intense itching and dry skin, suitable solutions can make daily management easier.
In this article, we explain everything about atopic skin: the definition of atopic dermatitis, the manifestations, the stages of the appearance of the disease, its biological origins, but also how to support it on a daily basis for greater well-being. be.
By observing your skin and its behavior, some signs can put you on the path to atopic dermatitis such as:
And if these manifestations appear episodically, in the form of alternating flare-ups and periods of remission , it is very likely that your skin is said to be atopic .
Also called eczema, atopic dermatitis is a chronic inflammatory disease, benign and non-contagious, with an allergic (immunological) component² .
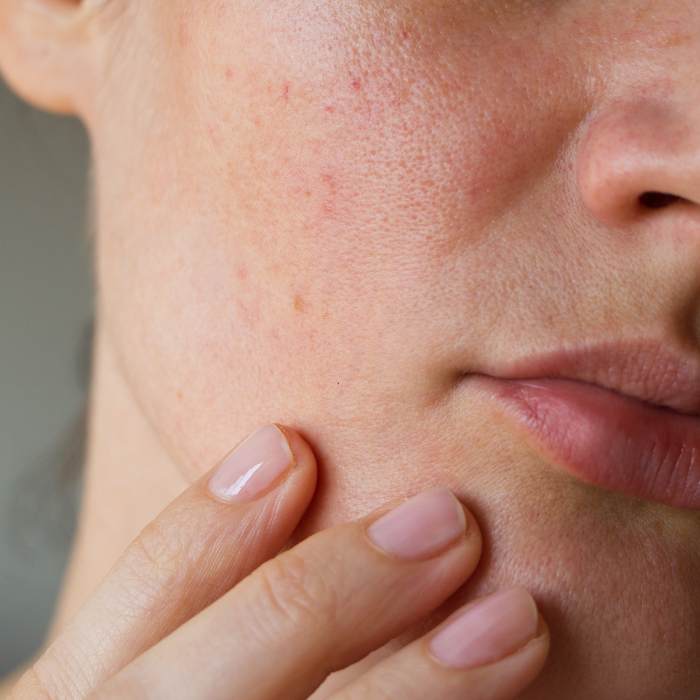
Although the symptoms are very similar (itching, redness, discomfort, etc.), atopic skin is not sensitive skin, nor reactive skin .
It is the allergic, or immunological, origin of atopic skin that distinguishes it from sensitive or reactive skin.
Sensitive and reactive skin is skin that reacts more or less intensely in the presence of factors that are aggressive to it (temperature variations, wearing clothes, cosmetic products, etc.) ³ .
In the presence of these factors, their tolerance thresholds are lower (almost zero for reactive skin) than in non-sensitive skin.
Unlike atopic skin, the hypersensitivity of sensitive and reactive skin is not induced by an allergic phenomenon, but rather by an alteration of the barrier function of the skin and a disruption of its nervous system .
To find out more about sensitive skin , discover our dedicated article.
Discover our range of expert sensitive skin care , HYDRA+.
Discover our expert range of care for intolerant skin , CALM+.
It itches ! It's impossible to miss it! Atopic dermatitis is essentially characterized by intense itching ; your doctor will surely tell you about skin pruritus . And it's very difficult to resist the urge to scratch. Although it is not painful, itching is nevertheless very uncomfortable , and causes significant discomfort on a daily basis . Insomnia and nighttime awakenings are frequently reported by people prone to atopic skin.
Other symptoms may put you on the path ⁴ :
Furthermore, atopic dermatitis is also associated with symptoms of other atopic diseases such as food allergies, asthma, allergic rhinitis and even conjunctivitis.

Atopic skin can affect the entire body and/or with more localized damage to:
However, we observe some differences in locations depending on the age of the infant, child and adult.
Research shows that atopic dermatitis has a genetic origin : in 50 to 70% [7] of people affected, a parent also has atopic skin.
Overall, atopic dermatitis is generally caused by a combination of several genetic, immune and environmental factors: ⁵
Atopic skin is characterized by extreme dryness . In question ? Defects in components essential to the structure of the skin and which guarantee the effectiveness of its barrier function. On the one hand, a deficiency in skin lipids , and on the other hand, a defect in the synthesis of an essential protein , filaggrin. By making the skin more permeable to its environment, these anomalies of genetic origin weaken the skin barrier. The deeper layers of the skin are then exposed to environmental influences, such as allergens or irritants present in the air or in the products we use. All of this can increase the sensitivity of the skin and make it react more easily and more intensely.
In the case of atopic dermatitis, the immune system reacts disproportionately in response to the presence of environmental allergens such as pollution , microorganisms , pollen , dust mites , animal hair ... This phenomenon leading to a chronic inflammatory reaction is all the more important as the permeability of the epidermis is high in atopic skin.
Recent scientific work tends to show that other potential factors contribute to atopic dermatitis :

As we have mentioned, atopic dermatitis is of allergic origin . That is to say, in the presence of allergenic components, the skin becomes allergic and sets up an inflammatory response (redness, discomfort, etc.).
Different types of allergens can trigger atopic dermatitis flare-ups:
Other irritating factors can also cause attacks such as heat , sweating or wearing clothing .
Atopic dermatitis is a progressive disease that generally begins very early, in infants. With age, it persists during childhood, and most of the time regresses in adulthood.
Atopic dermatitis begins to appear in infants, around the age of 3 months . However, it can occur from the first days of life. In infants, lesions develop mainly on plump areas of the face (particularly around the nose ), arms and legs , buttocks , but also on the scalp ⁶ .
Quite common in children, atopic dermatitis affects around 20% of children . Generally, atopic dermatitis in children [7] is localized more in folded areas such as the neck , elbows and knees . Lesions can also appear on the face and hands .
If atopic dermatitis tends to disappear during childhood (50% before 5 years), it is estimated that 10 to 15% of cases persist until adulthood. It is rare for atopic dermatitis to begin only in adulthood [8]. At this stage, the lesions are mainly located in the folds of the elbows and knees .
People suffering from eczema say it: they have to face many inconveniences in their daily life [5] with consequences that are sometimes difficult to live with :
The psychological impact of atopic dermatitis can affect the social life of those affected. If you are suffering, we advise you to seek help from a professional .
Although atopic dermatitis is a chronic skin condition, it is, however, possible to improve the daily life of atopic skin through certain practices that allow outbreaks to be spaced out and better managed, thus helping to live more peacefully with our atopic skin

It is important to diagnose atopic dermatitis from the first manifestations , at the infant stage. Indeed, it is observed that the first inflammatory outbreaks encourage new attacks, thus generating a bad vicious circle.
At the first suspicion, do not hesitate to quickly consult a general practitioner, a pediatrician or a dermatologist.
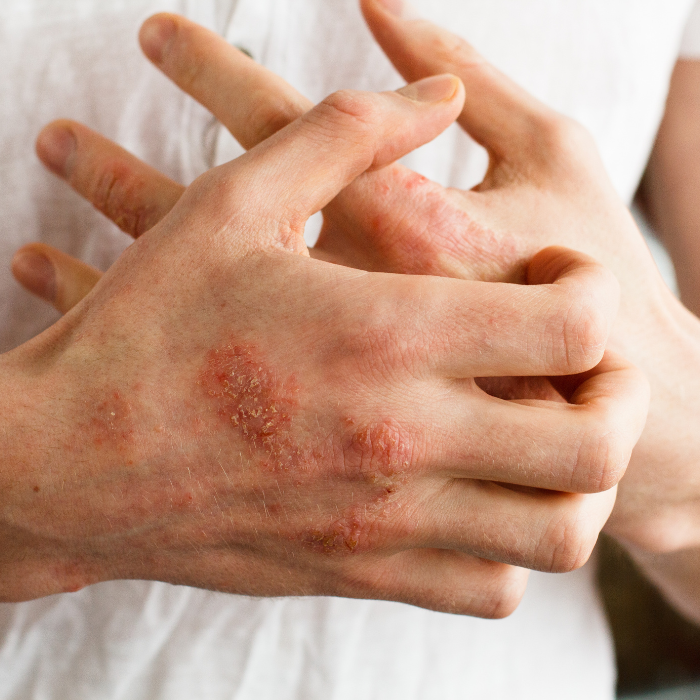
Depending on the severity of the symptoms, several solutions may be necessary in agreement with your doctor [9]:
Mild atopic dermatitis:
Moderate atopic dermatitis:
Severe dermatitis:

It is very important to intensely hydrate your skin, every day, with an emollient treatment . Milks, creams, balms... there is necessarily the right solution depending on the degree of dryness of your skin.
When washing , choose a very gentle cleanser , preferably without soap and with fatty substances, such as shower oils .
To help you find products suited to your atopic skin, here are some criteria to prioritize:
Finally, know that you can find advice and support from associations dedicated to patients affected by atopic dermatitis, such as the French Eczema Association . Our DA PROTECT face cream, cleansing oil and emollient body balm formulas have been tested and approved by this association.
Discover our range of expert care for atopic skin and atopic dermatitis , DA PROTECT.
TOPICREM formulas have all been designed to provide protective hydration and preserve the skin barrier of sensitive skin for the whole family.
To do this, our laboratory relies on its expertise derived from pharmaceutical excellence:
Through the comfort and emotional well-being they provide, our cares help you feel confident with your skin and with yourself, to better reveal yourself to others, and thus to fully enjoy every moment of life.
Bibliographic references:
¹ MA Richard et al. Prevalence of comorbidities in psoriasis and atopic dermatitis. Analysis based on the Objectifs Peau study. Annals of Dermatology and Venereology. Volume 144, Issue 12, Supplement, December 2017, Page S55
² Weidinger, S., & Novak, N. (2016). Atopic dermatitis. Lancet (London, England), 387(10023), 1109‐1122. https://doi.org/10.1016/S0140-6736(15)00149-X)
³ Ref: Misery L, Ständer S, Szepietowski JC, Reich A, Wallengren J, Evers AW, et al. Definition of sensitive skin: an expert position paper from the special interest group on sensitive skin of the IFSI (International Forum for the Study of Itch) Acta Derm Venereol. 2017;97:4-6.
⁴ Dharmage, SC, Lowe, AJ, Matheson, MC, Burgess, JA, Allen, KJ, & Abramson, MJ (2014). Atopic dermatitis and the atopic market revisited. Allergy, 69(1), 17‐27. https://doi.org/10.1111/all.12268
⁵ Dermato-Info.fr (information site of the French Society of Dermatology). Hives.
⁶ Weidinger, S., & Novak, N. (2016). Atopic dermatitis. Lancet (London, England), 387(10023), 1109‐1122. https://doi.org/10.1016/S0140-6736(15)00149-X)
7 Barbarot, S., Auziere, S., Gadkari, A., Girolomoni, G., Puig, L., Simpson, EL, Margolis, DJ, de Bruin-Weller, M., & Eckert, L. (2018) . Epidemiology of atopic dermatitis in adults: Results from an international survey. Allergy, 73(6), 1284‐1293. https://doi.org/10.1111/all.13401
[8] https://www.inserm.fr/dossier/dermatite-atopie-eczema-atopée/
[9] Wollenberg, A., Barbarot, S., Bieber, T., Christen-Zaech, S., Deleuran, M., Fink-Wagner, A., Gieler, U., Girolomoni, G., Lau, S ., Muraro, A., Czarnecka-Operacz, M., Schäfer, T., Schmid-Grendelmeier, P., Simon, D., Szalai, Z., Szepietowski, JC, Taïeb, A., Torrelo, A., Werfel, T., ... European Dermatology Forum (EDF), the European Academy of Dermatology and Venereology (EADV), the European Academy of Allergy and Clinical Immunology (EAACI), the European Task Force on Atopic Dermatitis (ETFAD), European Federation of Allergy and Airways Diseases Patients' Associations (EFA), the European Society for Dermatology and Psychiatry (ESDaP), the European Society of Pediatric Dermatology (ESPD), Global Allergy and Asthma European Network (GA2LEN) and the European Union of Medical Specialists (UEMS). (2018). Consensus-based European guidelines for treatment of atopic eczema (atopic dermatitis) in adults and children: Part I. Journal of the European Academy of Dermatology and Venereology: JEADV, 32(5), 657‐682. https://doi.org/10.1111/jdv.14891
Is your skin hot, tight, red? No doubt it is sensitive , as it is for more than half of the Frenc...
Read the article
If you want to spend more time with your skin, TOPICREM has a few tips for an uncomplicated routi...
Read the article
Discover how this simple ritual can enhance your skin, revealing its natural luminosity. From eli...
Read the article



